There is no universal definition for clinical significant prostate cancer, but the most frequent applied definition is the following: Pathology/histology with Gleason score ≥ 7 (including 3 + 4 with prominent but not predominant Gleason 4 component), and/or volume ≥ 0.5 cc, and/or extra prostatic extension (EPE).
Prostate cancer is divided into clinically insignificant and significant prostate cancer, depending on its likelihood to affect a patient’s lifetime. Prostate biopsies are assessed histologically by the Gleason score, a prognostic factor of prostate cancer, which provides information on tumour aggressiveness. Benign pathologies such as benign prostatic hyperplasia can raise PSA levels and normal PSA levels can not exclude prostate cancer. PSA is highly sensitive but not specific for prostate cancer. Prostate cancer screening is based on digital rectal examination (DRE) and prostate-specific antigen (PSA) level testing in the blood serum. According to two big screening studies “Prostate cancer screening in the randomized Prostate, Lung, Colorectal, and Ovarian Cancer Screening Trial” (PLCO) and “Screening and prostate cancer mortality: results of the European Randomised Study of Screening for Prostate Cancer” (ERSPC) overdiagnosis is common, therefore screening for prostate cancer is controversial.

The prevalence of latent prostate cancer at autopsy is high and occult carcinomas are common. Mortality of prostate cancer is difficult to measure due to the mortality of concomitant cardiovascular diseases and other cancers which share similar risk factors and therefore act as confounders. The incidence varies over a broad range among different countries probably as a result of a difference in the number of men screened. Two thirds of prostate cancer cases are diagnosed in the more developed regions of the world. Prostate cancer is the second most common cancer in men worldwide. Up to four suspicious lesions of category 3, 4 and 5 are assigned on a sector map and the index lesion should be identified. DCE-MRI has been attributed a minor role and only qualitative assessment with presence or absence of focal enhancement is suggested. The dominant sequence to detect prostate cancer in the peripheral zone is DWI, whereas for tumour detection in the transition zone T2w is the most important sequence.
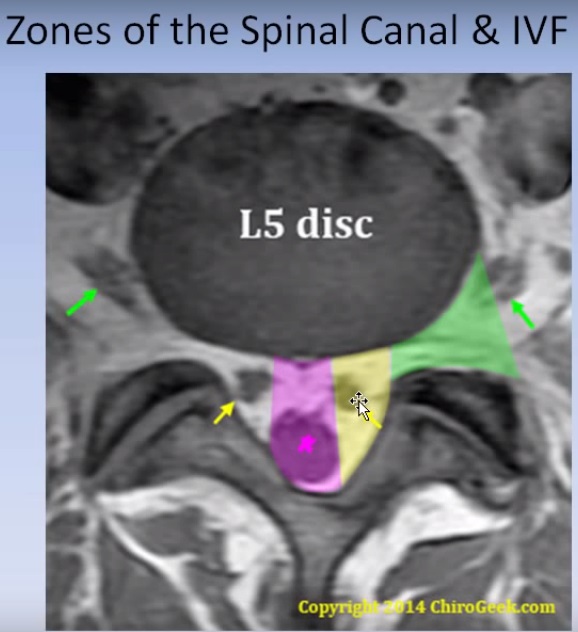
PI-RADS assessment categories range from 1 to 5 with 5 being most likely to represent clinically significant prostate cancer. Findings on mpMRI are assessed on a 5-point category scale based on the probability that a combination of findings on T2-weighted (T2w) sequences, diffusion-weighted MRI (DWI) and dynamic contrast-enhanced MRI (DCE-MRI) correlates with the presence of a clinically significant prostate cancer at a particular location. PI-RADS™ v2 improves and standardises communication between radiologists and urologists to detect or exclude the presence of significant prostate cancer with a high likelihood. It does not address detection of recurrence, progression during active surveillance and evaluation of other parts of the body. PI-RADS™ v2 aims to promote global standardisation, to diminish variation in the acquisition, interpretation and reporting of prostate mpMRI examinations and to improve detection, localisation, and risk stratification in patients with suspected cancer in treatment naïve prostate glands. Prostate imaging and interpretation is based on prostate imaging reporting and data system version 2 (PI-RADS™ v2) providing clinical guidelines for multiparametric magnetic resonance imaging (mpMRI) of the prostate.
